 Genetic testing can be both informative as well as an effective preventative method by locating specific pre-cursors to disease: genomic bio-markers. According to the U.S. National Library of Medicine, “Genetic testing has potential benefits whether the results are positive or negative for a gene mutation. Test results can provide a sense of relief from uncertainty and help people make informed decisions about managing their health care. For example, a negative result can eliminate the need for unnecessary checkups and screening tests in some cases. A positive result can direct a person toward available prevention, monitoring, and treatment options. Some test results can also help people make decisions about having children. Newborn screening can identify genetic disorders early in life so treatment can be started as early as possible.”
Genetic testing can be both informative as well as an effective preventative method by locating specific pre-cursors to disease: genomic bio-markers. According to the U.S. National Library of Medicine, “Genetic testing has potential benefits whether the results are positive or negative for a gene mutation. Test results can provide a sense of relief from uncertainty and help people make informed decisions about managing their health care. For example, a negative result can eliminate the need for unnecessary checkups and screening tests in some cases. A positive result can direct a person toward available prevention, monitoring, and treatment options. Some test results can also help people make decisions about having children. Newborn screening can identify genetic disorders early in life so treatment can be started as early as possible.”
Three of the most well-known abnormal genes are BRCA1, BRCA2, and PALB2. Women and men who inherit a mutation, or abnormal change, in any of these genes have a much higher-than-average risk of developing breast cancer and ovarian or prostate cancer. Continue reading
Tag Archives: Breast


What You Should Know About Breast Stereotactic Biopsy Procedures
If a Patient’s Breast MRI in Aventura Shows Abnormalities, a Breast Stereotactic Biopsy May be Needed
Breast MRI in Aventura is one of the most common diagnostic imaging tests performed in the area. When a patient’s results show abnormalities, further testing is often required in order to determine whether the area in question is benign or cancerous. Continue reading

What are the different types of breast cancer?
Although many of us think of breast cancer as a single disease, the diagnosis is not limited to one type. Most breast cancers start as small tumors. Some stay put; others travel. How the tumor behaves and how it grows will dictate how it’s classified and your treatment options.
The Cancer Treatment Centers of America website broadly organizes breast cancers into two groups based on how the cancer behaves: noninvasive (in situ) breast cancer and invasive (infiltrating) breast cancer.
Noninvasive Breast Cancers
In noninvasive breast cancer, “cancerous cells remain in a particular location of the breast, without spreading to surrounding tissue, lobules or ducts,” the website reports. Noninvasive breast cancers are generally earlier stage cancers that respond well to treatment. Ductal Carcinoma In Situ, or DCIS, is the most common form of noninvasive breast cancer; the American Cancer Society reports that 60,000 cases of DCIS, or about 20 percent of all breast cancer cases, are diagnosed in the United States each year.
DCIS begins inside the milk ducts – ‘in situ’ means that it stays within the duct and is considered noninvasive because it hasn’t spread to other surrounding tissues. Dr. Harold Burstein, institute physician at Dana-Farber Cancer Institute in Boston and associate professor of medicine at Harvard Medical School says it’s a “precancerous lesion, often diagnosed in women who’ve had mammograms, and it’s sort of a precursor to breast cancer.” Similar to a colon polyp. “It’s a benign growth, but you remove it to remove the growth” and prevent the development of invasive cancer.
Even with surgery to remove the growth, patients with SCIS are at higher risk of reoccurrence and later development of invasive cancer, but breastcancer.org reports the rate of reoccurrence is less than 30 percent.
Invasive Breast Cancers
In invasive breast cancers “cancerous cells break through normal breast tissues barriers and spread to other parts of the body through the bloodstream and lymph nodes,” reports Breastcancer.org. According to the American Cancer Society, invasive ductal carcinoma, or IDC, is the most common form of breast cancer – about 80 percent of cancer diagnoses are ISC and about 180,000 new cases are diagnosed each year in the U.S.
As with DCIS, IDC also begins inside the milk ducts, but these growths have moved beyond those boundaries and have begun invading or infiltrating the tissues around the ducts. Unlike noninvasive lesions, these growths are cancerous tumors, and treatment will likely be more aggressive than with a SCIS diagnosis. If left untreated, IDC usually spreads to the lymph nodes and then onwards to other parts of the body.
Get your yearly 3d mammogram and breast cancer screening at CBCC! Early detection is the best way to fight breast cancer. Call 800-371-0002 to schedule your appointment. The Center for Diagnostic Imaging in Miami also offers advanced MRIs, CT Scans, and more.

Breast Cancer: The Importance of Early Detection and Screening
Women in the United States have a 1 in 8 chance of getting breast cancer. The good news is that
when breast cancer is detected early, it can be cured. Studies show that the five-year survival rate for localized breast cancer is 97 percent, while the 12-year survival rate is 95 percent for cancers that are detected while still smaller than 1 centimeter in size. The size of the cancer and how much it has spread are two of the most important factors contributing to the success of treatment.
The key to successful treatment is early detection and screening. Screening exams are designed to find breast cancer while it is still small and localized – before it causes symptoms like an obvious lump. Breast cancers detected after symptoms arise are usually bigger and are more likely to have spread to areas beyond the breast. Early detection saves thousands of lives each year, so it’s important for women of all ages to know what tests are available and when to get them.
Women Ages 50+
Women in their 50s are at the greatest risk of contracting breast cancer. What are some ways to prevent it? Watch your weight! Women who gain weight (20 pounds or more ) after menopause are significantly more likely to be diagnosed with breast cancer than women who maintain a healthy weight.
Maintain at least a yearly mammogram to monitor any possible breast cancer developments.
Women Ages 40 – 49
Women 40 and older should have a mammogram each year, as long as they are healthy and free from serious health problems like congestive heart failure, end-stage renal disease, dementia, etc.
Various types of mammograms are available today, including 2D film or digital mammograms and 3D mammograms. Regardless of type, a mammogram is safe and is considered to be the best available test for detecting and diagnosing breast cancer.
Film, digital and 3D mammograms all use compression and a series of X-rays to generate pictures of internal breast tissue. During the exam, the technician compresses the breast with a paddle and takes images from various angles to obtain the necessary pictures.
If a patient receives abnormal mammogram results, doctors often order a breast ultrasound or an MRI breast scan as a follow-up test. These tests can zero in on a specific area identified by the mammogram, and they can help shed more light on whether the area in question might be a cyst or solid mass. A breast ultrasound or MRI breast scan can also sometimes distinguish between benign and cancerous tumors and can help doctors determine whether steps such as a stereotactic breast biopsy are necessary.
Women in 20s and 30s
Younger women – those in their 20s and 30s – should have clinical breast exams every three years. A CBE is usually done in conjunction with a mammogram and is an opportunity for women to discuss any changes in breast tissue, options for medical imaging scans, and any hereditary factors that could increase breast cancer risk.
A breast self-exam is another option for women starting in their 20s, and is something that can be done on a monthly basis throughout life. While self-exams play a smaller part in detecting breast cancer compared to other methods, they nonetheless help women become familiar with how their breasts normally look and feel. This makes it more likely that a woman will notice if a change occurs – perhaps a lump, swelling, pain, discharge, etc. Many times these symptoms are not cancerous, but they should always be reported to a doctor so the appropriate follow up tests can be done.
For a woman in her 20s, the odds of contracting breast cancer are quite low; however, the risk does increase with age. CBEs and self-exams enable women to know what is normal for them so they can immediately report any changes to their doctors.
High-Risk Women
Today, doctors use various risk assessment tools – such as the Gail model, the Claus model, and the Tyrer-Cuzick model – to help determine a woman’s risk for breast cancer. These tools give approximations of risk based on various factors and data. Genetic testing is also available and can identify whether a woman carries the BRCA1 or BRCA2 gene mutation.
For women who are identified as high-risk patients, experts recommend a yearly mammogram and MRI breast scan. An MRI breast scan is used in addition to a mammogram, rather than in place of it. While an MRI is more sensitive than a mammogram, it does miss some cancers that a mammogram can otherwise detect.
In most of these high-risk cases, the combination of mammograms and MRI breast scans should start at age 30 and continue as long as a woman is healthy enough to receive the tests. However, the age to start the exams should take personal situations and needs into account and can be modified accordingly by the doctor and patient.
Women having any of the medical imaging scans mentioned above should do so at a certified diagnostic imaging center to ensure they receive the most accurate tests possible. The Center for Diagnostic Imaging is proud to offer Comprehensive Breast Care Centers in the Miami area that offer all women access to life-saving mammograms, breast ultrasounds and MRI breast scans.

October is Breast Cancer Awareness Month
This month, we remind our patients to take steps to have a plan to detect breast cancer in its early stages and to encourage the women in your life to do the same. This plan can be as simple as performing regular breast self-exams and scheduling your clinical breast exams and mammograms based on your age and health history.
The American Cancer Society recommends that women without breast symptoms who are 40 and older should have a mammogram every year. Beyond mammograms, our CDI centers in South Miami and Aventura offer advanced Breast MRIs. MRI excels at imaging soft tissue and is therefore recommended for women with higher risk levels for breast cancer.
Is a Breast MRI Right for Me?
Use these guidelines developed by the American Cancer Society to help determine if you should talk to your doctor about a Breast MRI exam.
Recommended Annual Screening Indications
- BRCA1 – Women with this gene mutation have a 60-80% chance of developing breast cancer over a lifetime.
- BRCA2 – Women with this gene mutation have a 40-80% chance of developing ovarian cancer over a lifetime.
- Women with a first-degree relative who is a CRCA carrier, but who is untested.
- Women with a lifetime risk of breast cancer of 20-25% or greater.
- Women who have had radiation to the chest area between the ages of 10-30 (usually for Hodgkin’s Disease).
Diagnostic Indications
- Evaluation of suspicious clinical or imaging findings that remain indeterminate after a mammogram, ultrasound and physical exam
- Finding the extent of infiltrating ductal carcinoma and infiltrating lobular carcinoma
- Contralateral breast examinations in patients with breast malignancy
- Evaluation before, during and after neo-adjuvant chemotherapy
- Evaluation pre- or post-lumpectomy
- Suspected tumor recurrence in patients with or without post-operative tissue reconstruction
- Checking for breast malignancy with primary tumor unknown (MRI can usually see the exact location of a mass to save the breast)
- Checking for leakage in silicone augmentation (verify insurance coverage prior to exam)
If you need a Breast MRI or 3D mammogram, take advantage of our Comprehensive Breast Care Center (“CBCC”) for the best treatment options in South Florida. We specialize in early detection of breast cancer, provided by a fully trained staff and team of Board Certified Radiologists. With locations in North Miami Beach, South Dade, and Aventura, CBCC has South Florida covered when it comes to advanced breast cancer screenings. Call us at 1.800.371.0002 to schedule your appointment today.

MRI Links Saturated Fats to Breast Cancer in Postmenopausal Women
The presence of high saturated fatty acids in breast tissue may be a useful indicator of cancer in postmenopausal women, according to a new study by researchers at NYU Langone medical Center. The study was published online in Radiology, a journal of the Radiological Society of North America.
The researchers identified the relationship between fatty acids and breast cancer. Perhaps one day, these finding may lead to a greater understanding of the underlying mechanisms behind breast cancer development and the role of fat as a factor in breast cancer diagnosis and progression.
“Our study offers the first evidence — seen in breast tissue — that high saturated fatty acids in the breast adipose tissue is associated with presence of breast cancer in postmenopausal women,” said senior author and investigator Sungheon G. Kim, Ph.D., associate professor in the Department of Radiology at NYU Langone and a researcher at the Center for Advanced Imaging, Innovation and Research.
The relationship between body mass index (BMI), fat and cancer development has previously been studied, with postmenopausal women found to be at increased risk for breast cancer as their BMI increases. However, this study suggest the composition of the fat itself may play a role as well.
The relationship between body mass index (BMI), fat and cancer development has previously been studied, with postmenopausal women found to be at increased risk for breast cancer as their BMI increases. However, this study suggest the composition of the fat itself may play a role as well.

Breast cancer: Scientists discover genetic breakthrough.
The study, published in Nature, has been described as a “milestone” moment that could help unlock new ways of treating and preventing the disease.

Adding MRI to Mammography Could Help Detect Aggressive Breast Cancer
Breast imaging with magnetic resonance imaging (MRI) can detect a larger tumor burden than can mammography alone, which could impact treatment decisions, according to a study published in Radiology. The retrospective study demonstrated that of 2,021 newly diagnosed breast cancer patients, 285 patients (14%) had additional cancer detected by MRI, 73 of whom had cancers in a different quadrant of the breast than the index tumor.
Continue reading

Stereotactic Breast Biopsy
Stereotactic breast biopsy uses mammography – a specific kind of low-dose breast imaging that helps locate a breast lump or abnormality and remove tissue sample for examination under a microscope. It’s less invasive than surgical biopsy, leaves little to no scarring and can be an excellent way to evaluate calcium deposits or tiny masses that are not visible on ultrasound.
What is Mammographically Guided Breast Biopsy?
A breast biopsy is performed to remove suspicious area in the breast and examine them under a microscope. Suspicious areas may include:
- An unidentified mass
- Microcalcifications, a tiny cluster of small calcium deposits
- A distortion in the structure of the breast tissue
- An area of abnormal tissue change
- A new mass or area of calcium deposits is present at a previous surgery site
How should I prepare?
Before the exam, you may be asked to remove some or all of your clothes and to wear a gown during the exam. You will have to remove jewelry, dental appliances, eye glasses and any metal objects or clothing that might interfere with the x-ray images.
You should also report all medications that you are taking – including herbal supplements.
How is the procedure performed?
– Breast biopsies are usually done on an outpatient basis.
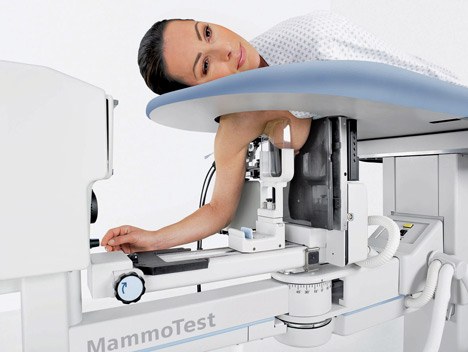
– In most cases, you will lie face down on a moveable exam table and the affected breast will be positioned into an opening in the table.
– The table is raised and the procedure is then performed beneath it. If the machine is an upright system, you may be seated in front of the stereotactic mammography unit.
– The breast is compressed and held in position throughout the procedure.
– Preliminary stereotactic mammogram images are taken.
– A local anesthetic will be injected into the breast to numb it.
– A very small nick is made in the skin at the site where the biopsy needle is to be inserted.
RadiologyInfo explains the pros and cons of this procedure:
Benefits:
– The procedure is less invasive than surgical biopsy, leaves little or no scarring and can be performed in less than an hour.
– Stereotactic breast biopsy is an excellent way to evaluate calcium deposits or masses that are not visible on ultrasound.
– Stereotactic core needle biopsy is a simple procedure that may be performed in an outpatient imaging center.
– Compared with open surgical biopsy, the procedure is about one-third the cost.
– Very little recovery time is required.
– Generally, the procedure is not painful.
– No breast defect remains and, unlike surgery, stereotactic needle biopsy does not distort the breast tissue and make it difficult to read future mammograms.
– Recovery time is brief and patients can soon resume their usual activities.
– No radiation remains in a patient’s body after an x-ray examination.
– X-rays usually have no side effects in the typical diagnostic range for this exam.
Risks:
– There is a risk of bleeding and forming a hematoma, or a collection of blood at the biopsy site. The risk, however, appears to be less than one percent of patients.
– An occasional patient has significant discomfort, which can be readily controlled by non-prescription pain medication.
– Any procedure where the skin is penetrated carries a risk of infection. The chance of infection requiring antibiotic treatment appears to be less than one in 1,000.
– Depending on the type of biopsy being performed or the design of the biopsy machine, a biopsy of tissue located deep within the breast carries a slight risk that the needle will pass through the chest wall, allowing air around the lung that could cause the lung to collapse. This is an extremely rare occurrence.
– There is always a slight chance of cancer from excessive exposure to radiation. However, the benefit of an accurate diagnosis far outweighs the risk.
– Women should always inform their physician or x-ray technologist if there is any possibility that they are pregnant. See the Safety page for more information about pregnancy and x-rays.
As medical imaging technology continues to advance, it is important to stay informed of the latest treatments so that your healthcare can become simpler and easier. Schedule your exam today and benefit!

FDA Approves Cap to Prevent Hair Loss During Chemo

Hair loss is one of the most despised side effects of chemotherapy, and new technology is now offering a way to save those precious locks.
Continue reading