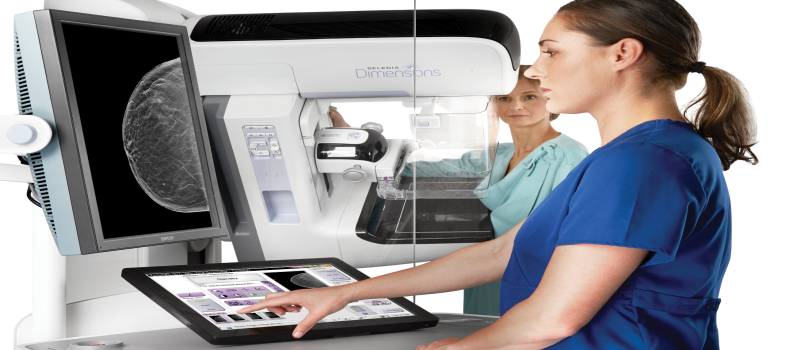
There are several new developments afoot in the medical imaging world. Trends such as: multidisciplinary teams, big data, tomosynthesis, and patient engagement, among others. These themes gained traction through highly publicized research, making 2015 an exciting year for diagnostic imaging. According to Norman Yung, Chief Marketing Officer of Carestream, “Last year marked the time when certain trends were shown to have benefits, and this year will be the time when these ideas are put into practice among a larger portion of the industry.” Continue reading
There are several new developments afoot in the medical imaging world. Trends such as: multidisciplinary teams, big data, tomosynthesis, and patient engagement, among others. These themes gained traction through highly publicized research, making 2015 an exciting year for diagnostic imaging. According to Norman Yung, Chief Marketing Officer of Carestream, “Last year marked the time when certain trends were shown to have benefits, and this year will be the time when these ideas are put into practice among a larger portion of the industry.” Continue reading
Tag Archives: 3D mammography


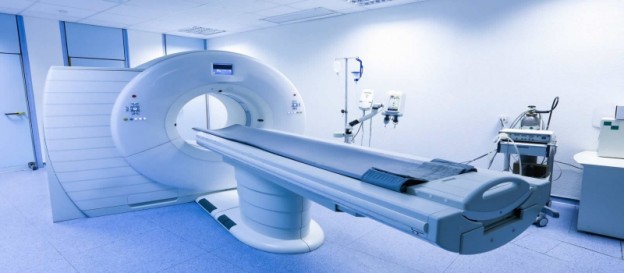
Why 3D Mammography Should be Covered by Insurers
3D Mammography is FDA Approved and Offers Many Benefits over Traditional Mammograms
There have been rumors in the healthcare industry that insurance carriers would finally start to cover tomosynthesis (3D mammograms), in addition to traditional 2D film or digital mammograms. Unfortunately, we have yet to see these rumors come to fruition, at least not on a widespread basis.
To date, most insurers refuse to pay for a patient’s 3D mammogram, citing reasons such as the technology is “too new,” “unproven,” or “not medically necessary.” At the Center for Diagnostic Imaging in Miami, we strongly disagree with this rationale and believe it is time for insurers to step up and start providing coverage for 3D mammography. Here is why:
1. Tomosynthesis provides earlier and easier breast cancer detection. A traditional mammogram provides only two dimensional views of breast tissue in a flat image. The tissue often appears overlapped, making it difficult to see all the individual internal structures. 3D mammography solves this problem by allowing radiologists to better see the structures and tissues of the breast. It is 40 percent more sensitive than a 2D mammogram, so it is better at detecting small cancers, multiple abnormalities, and the exact size, shape and location of possible cancers. This is particularly beneficial for women with dense breast tissue or for those at high risk for breast cancer.
2. 3D mammography results in fewer false positives. Traditional mammograms often identify questionable areas of the breast that require additional diagnostic tests in order to identify or rule out cancer. Using a 3D mammogram to view the breast tissue in smaller, thinner sections prevents radiologists from having to call patients back for a “second look.” This saves time and keeps patients from agonizing over false alarms.
3. 3D mammograms are FDA approved. The FDA approved 3D mammography in 2011, and it is now available throughout the U.S.
4. Tomosynthesis is not new. In fact, it has been around for several decades. Some variants of tomosynthesis imaging were developed as early as the 1970s and 1980s, so it should not be considered a “new” imaging technology.
At the Center for Diagnostic Imaging, we believe so strongly in the benefits of 3D mammography that we became the first imaging center in South Florida to offer the technology for breast cancer screening. We urge all health insurance companies to reconsider their stand on tomosynthesis and finally provide coverage for this important, lifesaving test.

Why Do You Need A 3d Mammography?
Early detection of any cancer increases the probabilities of recovery by successfully treating it. Every woman in her mid-30s should get an annual mammogram for early detection of breast cancer.
A 3D mammogram (breast tomosynthesis) is the latest imaging test that combines multiple breast X-rays (like traditional mammography) for creating a three-dimensional image of the breast tissues for detecting any signs or symptoms of breast cancer or any other abnormalities. It is used to examine the reason for various breast problems, such as lumps, nipple discharge, and pain. 3D mammography produces highly detailed images of breast tissue by 3D capture of multiple slices of the breast from different angles.
The 3D mammogram takes approximately 300 images, giving an exact idea of the issue whereas two-dimensional mammogram takes about four images at a time giving some false alarms. It lets the radiologist view the breast tissue in full detail, equipping them to give a certain diagnosis, if they have cancer or not by visiting the nearest diagnostic center. This is specifically valuable for women with dense breast tissue, as they are at higher cancer risk.
Why is 3D Mammography Performed?
We know that traditional mammography took only two images of each breast of a side-to-side view and a top-to-bottom view. 3D mammography takes various X-ray images of the breasts from multiple angles to create a digital version of internal breast tissue. The multiple images make radiologists assess the breast in 1mm slices in place of only two views.
Radiologists correctly interpret results from 3D mammography in dense breast tissue, resulting in fewer false-positive and false-negative readings.
What to Expect from 3D Mammography
The preparation of a 3D mammography is exactly the same for traditional mammography. Women should schedule mammography at a date one week after their menstrual period starts because they are least tender at that time.
3D mammography involves a bare torso, so it is suggested to wear comfortable, easy-to-remove clothes. Avoid applying Deodorant, perfume, lotion, and other products on underarm or torso before 3D mammography, since these products interfere with the imaging process. Women should inform their radiologist or physician if they are pregnant, breastfeeding, have breast implants or suffer from any medical conditions, so they can change the procedure accordingly.
A radiologist interprets the results of 3D mammography by viewing the calcification or masses in the breast tissue and using a standardized classification system called Breast Imaging Reporting and Data System (BI-RADS).

Medical imaging- a key to patient healthcare
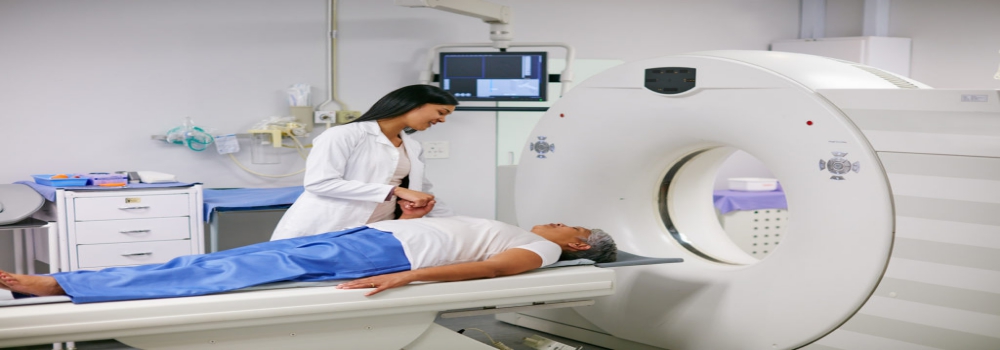
Medical imaging is extremely important as it helps in the prevention of many chronic diseases such as cancers and tumors. The doctors can detect, diagnose, and start the treatment as early as possible to prevent the patient from fatal diseases.
Diagnostic medical imaging uses a number of non-invasive methods that allows the radiologists and other medical personnel to see through the body and diagnose the underlying problem. Various organs and areas inside the body can be seen and treated with the help of medical imaging. It plays a crucial role in the healthcare of the patient.
Why medical imaging is one of the top developments in the face of clinical medicine?
It literally saves the life of a patient: The advancement in medical imaging has enhanced the screening of diseases and helps in the early diagnosis of acute and chronic conditions. In the absence of medical imaging, many of the severe and life-threatening diseases may go unnoticed until they reach a much more fatal stage.
Medical imaging has reduced the requirement for intrusive exploratory surgery: The development of technologies such as Magnetic Resonance imaging (MRI), Computed Tomography Scan (CT scan), and Echocardiography, x-ray services etc. has dramatically reduced the need for surgeries.
A huge amount of money is saved: With the right scan at the right time, the patient is able to get the proper treatment, thus costs as well as time is saved. As it replaces the need of surgery and also decreases the amount of time the patient has to remain in the hospital, so less cost is incurred for the treatment as well.
The doctors are able to identify the exact underlying problem that is causing the abnormal symptoms in the body and are able to give the proper treatment based on the reports of the patient.
Which tests involve ionizing radiation that might have a harmful effect?
There are generally four types of technologies that are used in medical imaging namely x-rays, MRI, Ultrasound, and nuclear medicine. The patient will be exposed to radiation depending upon the type of test carried out.
X-rays, 3d mammography, and fluoroscopy give out lesser radiation than the CT scans. The MRI and ultrasound do not emit any radiations as these can harm the children who are more sensitive to the radiation. The risks involved in medical imaging are less.
However, you should go for the imaging that is required to examine the exact condition. The benefits provided by medical imaging outweigh the risks associated with it.

The Importance of Mammograms
Breast cancer is the most commonly diagnosed cancer in women. One in eight women will be diagnosed with breast cancer in their lifetime. One of the most effective ways to find and/or prevent breast cancer is through regular mammography screenings.
A mammogram is a specific type of breast exam that uses a non-invasive X-ray process that doctors use to identify and treat any abnormal areas that may possibly indicate the presence of cancer. Annual mammograms can detect cancer up to two years before a patient or physician will notice any abnormalities. Mammograms can also prevent the need for extensive treatment for advanced cancers and improve chances of breast conservation.
The Miami Center for Diagnostic Imaging now uses an even quicker and more accurate version of digital mammography. 3D mammography, also called breast tomosynthesis, is a revolutionary technology that gives radiologists the ability to identify and characterize individual breast structures without the confusion of overlapping tissue. During a tomosynthesis scan, multiple, low-dose images of the breast are acquired at different angles. These images are then used to produce a series of one-millimeter thick slices that can be viewed as a three dimensional reconstruction of the breast.
Mammograms play an important role in women’s health. They have been shown to lower the risk of dying by 35% in women over the age of 50. Breast cancer is the second leading cause of death among women; it is estimated that over 220,000 women in the United States will be diagnosed; and an estimated 2,150 men will also be diagnosed. More than 80% of breast cancers are found in women with no family history.
In addition to mammograms, women, starting at the age of 20, should make sure to schedule regular clinical exams with a health care provider; and should also perform regular self-examinations. Women at average risk for developing breast cancer should discuss with their health care provider the potential benefits of a screening breast MRI in addition to their yearly mammogram.
The digital mammography experts at the Center for Diagnostic Imaging and Comprehensive Breast Care Centers provide women with the most advanced care available to help keep them healthy.
About Center for Diagnostic Imaging:
The Center for Diagnostic Imaging Miami staff is dedicated to providing the highest level of efficient and excellent care for each patient who walks through their door. The center, known for their reputation as one of the best full body scan Miami facilities in the state, is owned and managed by physicians, radiologists, technicians, and other highly trained and qualified staff. The staff-ran facility’s mission is to serve the healthcare needs of the Miami community with the use of the most highly advanced technology medical equipment within the diagnostic imaging industry.
With this type of technology available at their fingertips, staff members have the ability to better identify any issues or concerns impacting the health and well-being of each individual patient.
The Center for Diagnostic Imaging currently offers the following scanning services:
- Computer tomography Scan (CAT Scan)
- Computed Tomography Angiography Scan (CTA Scan)
- Magnetic Resonance Angiography scan (MRA)
- Magnetic Resonance Imaging (MRI)
- Nuclear Medicine
- Position Emission Tomography Scan (PET Scan)
- X-Rays
In addition to their diagnostic services, the center is also known as one of the most preferred breast ultrasound Miami facilities. When it comes to breast exams women the can receive 3D Mammography scans, MRI guided biopsies, and stereotactic biopsies.

Demystifying the Differences between 2D and 3D Mammography
Every year over 200,000 women in the U.S. are diagnosed with breast cancer, and every year breast cancer that has spread from the breast to other parts of the body (“late stage” or “metastatic” breast cancer) kills about 40,000 women. When breast cancer is detected early—before it has spread—it is easier to treat and women have a much better chance of surviving breast cancer. For now, mammograms are the best way of screening women for breast cancer.
In the United States, tomosynthesis – another name for 3D mammography – has been available in leading breast care centers since 2011. The FDA originally approved 3D mammography to be used in conjunction with 2D (digital) mammograms for breast cancer screenings. However, the agency determined last year that a 3D mammography system is now accurate enough to be used as a standalone test.

3D mammography generates images of the breast using technology similar to CT scans. Unlike 2D digital or film mammograms – which compress the breast and take images from only the front and side – a 3D imager takes multiple X-rays while moving across the breast in an arch. A computer then compiles the X-rays into a 3D reconstruction of the breast that can be analyzed by a radiologist. It takes just a few seconds longer than 2D mammograms, so the amount of radiation exposure is about the same. Patients generally experience no difference in the level of physical discomfort between 2D and 3D mammograms.
3D mammography has been a significant breakthrough in digital medical imaging. Unlike 2D mammograms that can obscure some cancers due to compressing and overlapping breast tissue, 3D mammography enables digital medical imaging specialists to examine breast tissue a layer at a time. A 3D mammogram is up to 40 percent more sensitive than digital or film mammograms, which means it can give doctors a clearer, more accurate picture of breast tissue and abnormalities.
3D mammograms can also be especially helpful for women with dense breast tissue as it’s more difficult to identify cancer in dense breasts. On a regular 2D mammogram, cancer and dense tissue appear almost the same, while a 3D mammogram can make better distinctions between the two.
The Center for Diagnostic Imaging is proud to provide patients and referring doctors with a comprehensive breast care center that has one of the only 3D mammography machines in the Miami area. We encourage all women to speak with their doctors right away if they experience any symptoms or suspect they are at high risk for breast cancer. Digital medical imaging plays an important role in the early detection and treatment of breast cancer.

How Dense Breasts Can Impact Breast Cancer Screening
and How 3D Mammography Offers Improved Accuracy
In some of our recent blogs, we have discussed how 3D mammography can be more accurate in detecting breast cancer in women with dense breasts. But, what exactly does it mean to have dense breasts?
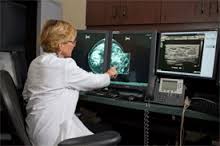
A doctor examines a digital mammogram of a dense breast and points to a potential cancer
Source: National Cancer Institute
Breast density refers to the ratio of fatty tissue to breast tissue – dense breasts have more breast tissue and less fatty tissue. Usually, the younger a woman is, the denser her breasts are, and the more difficult it is to “see” through the tissue on a mammogram to identify cancer. In fact, this is why mammograms are generally not done until a woman is 40, unless there is a history of breast cancer in her family. However, age is not the only factor. Some women can have naturally dense breasts their entire lives. About 1/3 of women over the age of 50 still have dense breasts. Continue reading

3D Mammography Increases Odds of Detecting Breast Cancer
Breast cancer awareness campaigns have heightened awareness of the importance of getting mammograms. However, there are big differences in mammography technology today.
Three-dimensional mammography, first approved by the FDA in 2011, known more specifically as digital breast tomosynthesis, detects 41 percent more invasive breast cancers that traditional mammograms.
Benefits to Patients
With no added demand on a patient’s time during an exam, 3D imaging can:
- Improve diagnostic confidence
- Replace more invasive and expensive diagnostic procedures, reducing risk of complications
- Minimize exploratory surgery
- Facilitate non-invasive surgical planning
- Reduce operating time
- Minimize damage to healthy tissue by targeting the treatment area
- Serve as easy-to-read visuals for patient education and communication.
| Share |
|

Mammography Trends to Watch This Year
A new year brings much in tow – new ideas to share, new trends to address, new technologies to install. While it is difficult to say exactly what will affect us the most as we begin 2017, there are certain trends that seem to leap out ahead of others. Here are five trends we expect to have a vital impact on medical imaging in 2017:
1. 3D mammography. Digital breast tomosynthesis (DBT) has been a frequent topic in trade publications for a few years. As more studies are released touting the success of this technology in finding lesions and reducing recall rates, its popularity is only going to increase. Especially as media has been touting the benefits of this technology in recent years.
2. Multimedia enhanced radiology reporting (MERR). Text-only reports are fading away. A study from Emory University and the Harvey L. Neiman Health Policy Institute found that 80% of respondents said MERRs “improved understanding of radiology findings by correlating images to text reports.” The study also found that the multimedia reports provided easier access to images while monitoring the progression of a condition, and saved time understanding findings without supporting images. While improving the radiology report, the multimedia-enhanced version also provides more financial value to radiologists.
3. Radiology goes to the cloud. Radiology is quickly migrating to the cloud. According to an article in Applied Radiology, the global cloud computing market in healthcare was valued at $1.8 billion in 2011, and is expected to grow at 21% at compounded annual growth rate (CAGR) of 21% to $6.8 billion by 2018. While initial upfront costs can vary between the intensity of building an organization’s own private cloud, or the ease and flexibility of using public cloud architecture, the process efficiency, financial predictability of paying for only what the organization needs and long-term cost savings are making the cloud a worthwhile investment.
4. Telemedicine. The global telemedicine market was $27 billion, and the market has already surged past that number for 2017. By 2018, two-thirds of interactions with healthcare organizations will be conducted via mobile devices. Last year was an important year for telemedicine, as wearable technology become prominent. Telemedicine is expected to be valued around $3.8 billion by 2019, according to Transparency Market Research. Expect telemedicine to bring together health facilities like never before – from large systems to those located in rural areas.
5. Centralization of clinical data. Collaboration is a must for health facilities. No department can be left out of the patient experience equation now.

Mammograms Are for Every Age
Women who think they are too old to worry about mammograms may want to reconsider the age at which their breast cancer screening years are behind them, a new study suggests.
Based on an analysis of nearly 7 million mammograms over a seven-year period, “the benefit continues with increasing age up until 90,” said study author Dr. Cindy Lee. She is an assistant professor in residence at the University of California, San Francisco.
The question of when to stop having mammograms has been widely debated. In 2009, the U.S. Preventative Services Task Force issued new guidelines, saying there wasn’t enough evidence to assess the balance of benefits and harms of screening mammography in women aged 75 and older.
According to the study, investigators looked to see whether the mammography screening correlated in higher cancer detection rate and a lower recall rate.
In the analysis, which included data from 39 states from 2008 through 2014, nearly four breast cancers were found for every 1,000 patients screened. The recall rate was 10 percent.
“We are finding more cancers with increasing age,” Lee said, which makes sense because the risk rises with age. “We are doing better at catching them,” she said. And, “we have decreased the recall rate. We are calling back fewer women for additional testing, but are finding more cancers.”
The study findings suggest that the decision to screen may depend on a woman’s personal choice and health status. The study was to be presented at the Radiolofical Society of North America annual meeting, in Chicago. Studies presented at medical meetings are viewed as preliminary until they are published in a peer-reviewed journal.
According to Robert Smith, vice president of screening for the American Cancer Society, said the study finding show that mammograms are still worthwhile after the age of 70.
“Many of these deaths are avoidable, as Lee and colleagues demonstrate in this new report, since mammography screening performs increasingly well as women get older. While incidence is high, the disease is slower growing and density is lower, providing improved opportunity for early detection,” Smith explained.
The Comprehensive Breast Care Centers in South Florida offer mammograms and 3D mammograms which help detect breast cancer early. Contact us today to schedule your Breast Cancer Screening and mammogram.