Stereotactic breast biopsy uses mammography – a specific kind of low-dose breast imaging that helps locate a breast lump or abnormality and remove tissue sample for examination under a microscope. It’s less invasive than surgical biopsy, leaves little to no scarring and can be an excellent way to evaluate calcium deposits or tiny masses that are not visible on ultrasound.
What is Mammographically Guided Breast Biopsy?
A breast biopsy is performed to remove suspicious area in the breast and examine them under a microscope. Suspicious areas may include:
- An unidentified mass
- Microcalcifications, a tiny cluster of small calcium deposits
- A distortion in the structure of the breast tissue
- An area of abnormal tissue change
- A new mass or area of calcium deposits is present at a previous surgery site
How should I prepare?
Before the exam, you may be asked to remove some or all of your clothes and to wear a gown during the exam. You will have to remove jewelry, dental appliances, eye glasses and any metal objects or clothing that might interfere with the x-ray images.
You should also report all medications that you are taking – including herbal supplements.
How is the procedure performed?
– Breast biopsies are usually done on an outpatient basis.
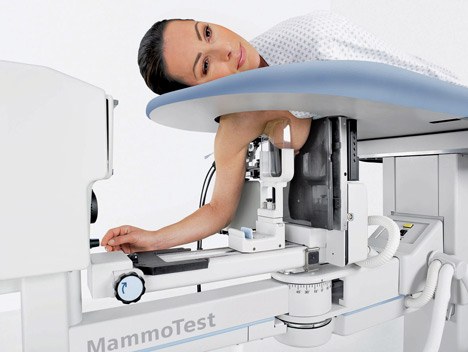
– In most cases, you will lie face down on a moveable exam table and the affected breast will be positioned into an opening in the table.
– The table is raised and the procedure is then performed beneath it. If the machine is an upright system, you may be seated in front of the stereotactic mammography unit.
– The breast is compressed and held in position throughout the procedure.
– Preliminary stereotactic mammogram images are taken.
– A local anesthetic will be injected into the breast to numb it.
– A very small nick is made in the skin at the site where the biopsy needle is to be inserted.
RadiologyInfo explains the pros and cons of this procedure:
Benefits:
– The procedure is less invasive than surgical biopsy, leaves little or no scarring and can be performed in less than an hour.
– Stereotactic breast biopsy is an excellent way to evaluate calcium deposits or masses that are not visible on ultrasound.
– Stereotactic core needle biopsy is a simple procedure that may be performed in an outpatient imaging center.
– Compared with open surgical biopsy, the procedure is about one-third the cost.
– Very little recovery time is required.
– Generally, the procedure is not painful.
– No breast defect remains and, unlike surgery, stereotactic needle biopsy does not distort the breast tissue and make it difficult to read future mammograms.
– Recovery time is brief and patients can soon resume their usual activities.
– No radiation remains in a patient’s body after an x-ray examination.
– X-rays usually have no side effects in the typical diagnostic range for this exam.
Risks:
– There is a risk of bleeding and forming a hematoma, or a collection of blood at the biopsy site. The risk, however, appears to be less than one percent of patients.
– An occasional patient has significant discomfort, which can be readily controlled by non-prescription pain medication.
– Any procedure where the skin is penetrated carries a risk of infection. The chance of infection requiring antibiotic treatment appears to be less than one in 1,000.
– Depending on the type of biopsy being performed or the design of the biopsy machine, a biopsy of tissue located deep within the breast carries a slight risk that the needle will pass through the chest wall, allowing air around the lung that could cause the lung to collapse. This is an extremely rare occurrence.
– There is always a slight chance of cancer from excessive exposure to radiation. However, the benefit of an accurate diagnosis far outweighs the risk.
– Women should always inform their physician or x-ray technologist if there is any possibility that they are pregnant. See the Safety page for more information about pregnancy and x-rays.
As medical imaging technology continues to advance, it is important to stay informed of the latest treatments so that your healthcare can become simpler and easier. Schedule your exam today and benefit!